Heart Disease Deaths during COVID: Not so Mysterious but Questions Remain
A recent Bloomberg headline reported: “A Spike in Heart Disease Deaths Since Covid Is Puzzling Scientists.” Cardiovascular deaths have been elevated during the pandemic, the article notes, and as others have previously described.
“Scientists are still trying to figure out why,” it asserts, noting that “[i]t’s unclear how many people died from Covid’s cardiovascular complications and how many died because of its indirect consequences, such as disrupted medical care and worsening rates of obesity and high blood pressure.”
But how mysterious is the spike in heart disease deaths really? My quick look at the data suggests that the culprit is mostly acute COVID-19.
The figures in the Bloomberg article are age-adjusted annual death rates. Instead, I looked at monthly multiple-cause-of death data from CDC WONDER, examining the number of deaths by month from 2018-2022 with “ischemic heart disease” (IHD) on the death certificate, which includes acute illnesses like heart attacks. I also looked at deaths with COVID-19 on the death certificate, and with both COVID and IHD (“IHD with COVID”) on the death certificate. I then subtracted COVID deaths from “IHD with COVID” deaths, to produce a monthly figure on “IHD without COVID” deaths, i.e. deaths where IHD was on the death certificate but not COVID.[1] Finally, I averaged monthly CV deaths pre-pandemic (2018-2019) which I compared to post pandemic counts.
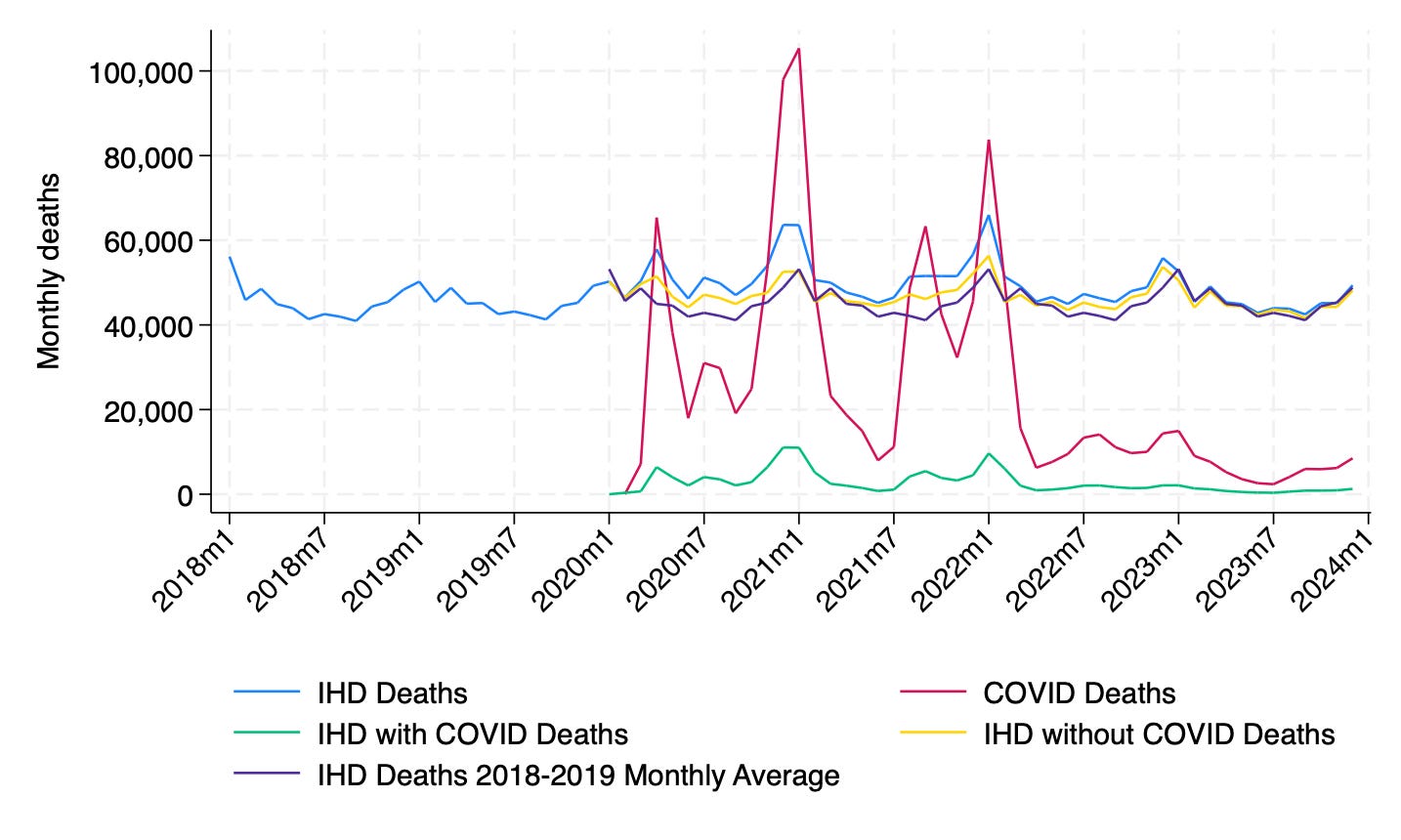
The figure below plots monthly counts of deaths for all five of these categories of deaths.
There are a few things to note. First, pre-COVID, note the wintry peaks in IHD deaths. This is not a novel observation: influenza / viral respiratory season (winter) has long been shown to be a time when deaths increase from various causes, including cardiovascular disease. Again, nothing new here, but an important reminder of the role that respiratory viruses play in “winter mortality” even for deaths not per se coded as pneumonia or influenza (although in my dataset, individuals could have had such additional codes).
Second, note that, during the pandemic, peaks in IHD deaths correspond closely with COVID peaks, for instance during the first big spring 2020 surge, the smaller summer surge that year, the bad 2020-21 COVID winter, and the double-humped delta-omicron summer 2021 - winter 2021/22 surge. In other words, the “unexplained” increases in IHD deaths spike at the same time as COVID deaths were surging. Similarly, between peaks of acute COVID deaths, IHD deaths drop closer to, but still somewhat above, their pre-pandemic baseline (at least until 2023). This is consistent with IHD deaths being driven by acute COVID.
Similarly, look at the line for “IHD without COVID deaths”. Again, these are deaths of individuals who have IHD but not COVID on their death certificate. This line appears much closer to the pre-pandemic average IHD deaths.
Finally, consider average differences in monthly deaths pre- and post-pandemic.
There were 45,299 monthly IHD deaths on average pre-pandemic (2018-2019) and 49,490 post-pandemic (2020-2022) — a monthly average difference of 4,191.
On the other hand, after excluding IHD deaths where COVID also appeared on the death certificate, we have 45,299 and 46,749 average monthly IHD deaths pre- and post-pandemic, respectively — a difference of 1,450.
In other words, roughly two-thirds of the average monthly excess IHD deaths post-pandemic go away once you exclude IHD deaths where COVID is also on the death certificate. This doesn’t even account for IHD deaths among those with acute COVID that was never diagnosed or was diagnosed but, for whatever reason, left off the death certificate.
This is admittedly a preliminary and simple analysis. I do not account for secular change in population size or age structure, which might be expected to produce some excess deaths in overall IHD deaths, or prevailing trends in death rates which should lower it. Such more sophisticated analyses are needed. However, this descriptive look at the data presents a reasonably clear picture to my mind.
Monthly excess IHD deaths in the pandemic era coincide with COVID waves but are also mostly accounted for by individuals who died of acute COVID (at least as a contributing factor). In contrast, there could be some late/post-acute COVID cardiovascular mortality, but if so, it is a much smaller factor, particularly given “IHD without COVID deaths” tended to return to the pre-pandemic IHD death baseline after surges, at least after 2020. Indeed, by 2023, monthly IHD deaths appear similar to the pre-pandemic average throughout the year.
This does leave some questions unanswered, however. In particular, what was the nature of the deaths of those with both IHD and COVID on the death certificate? There are two primary possibilities as I see it.
First, there are the sorts of patients who I treated throughout the pandemic: people who contracted COVID, developed severe pneumonia, and then progressed to multiple organ failure, which might include any number of cardiovascular complications that might appear on the death certificate along with COVID (as would codes for pre-existing heart disease if it was thought to be a contributing factor in the death). This is a scenario that is unfortunately not uncommon in critical care medicine: one severe illness culminates in a multitude of other organ failures and complications, which can include a heart attack.
Second, we can envision a patient who had a mild acute COVID infection and then, say, a heart attack out of the blue. This is an entirely different clinical scenario, even if, in both cases, both COVID and IHD appear on the death certificate.
These data do not allow us to differentiate these two types of patients. My suspicion is that the former type — the critically ill patient with severe COVID-19 pneumonia and many complications — characterizes the bulk of these deaths, particularly given that we see falling counts of “excess” IHD deaths during the pandemic despite ongoing high levels of infection, but further work would be necessary to make that conclusion. But this is an important clinical and policy issue. Are cardiovascular deaths in the setting of respiratory viral infections the consequence predominantly of severe respiratory disease, or of even a mild upper respiratory tract infection? That question has potential implications for how we should focus our efforts to mitigate harm.
[1] CDC WONDER suppresses cells with death counts < 10. This was the case for COVID deaths in January 2020 (which I do not plot) but also IHD with COVID deaths for February 2020. Given that the 1-9 count is a minuscule fraction of the 46,456 overall CV deaths that month, I disregarded these deaths for my IHD without COVID count for that month to ensure that I had an even number of observations of each calendar month both pre and post-pandemic.